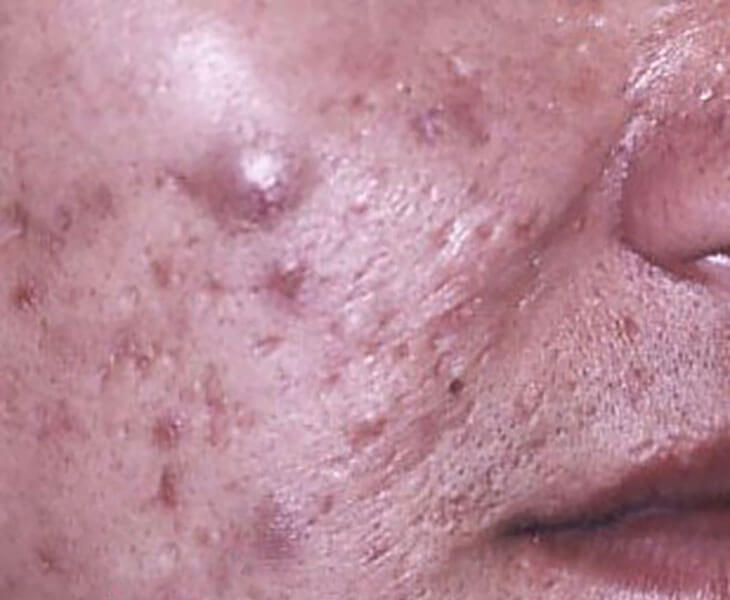
Is Your Acne Comedonica Cosmetic-Induced? Know the Signs
Living with persistent skin breakouts can be frustrating, especially when you’re meticulously caring for your complexion. If you’re experiencing a flurry of small, non-inflammatory bumps, you might be dealing with Akne Comedonica. But what if the very products you use to enhance your skin’s appearance are contributing to the problem? This article will delve into the world of Akne Comedonica, explore its close link to cosmetic products, and equip you with the knowledge to identify and manage this common skin concern.
Often referred to as “comedonal acne,” Akne Comedonica is a mild form of acne vulgaris primarily characterized by the presence of comedones—those pesky blackheads and whiteheads that give your skin a rough, uneven texture. While genetics and hormonal fluctuations are common culprits for acne, a significant and often overlooked trigger for Akne Comedonica can be found right in your daily skincare and makeup routine. This phenomenon is known as Acne Cosmetica or Acne Venenata, highlighting the crucial role cosmetics can play in skin health.
What Exactly is Akne Comedonica? Unpacking the Comedone
At its core, Akne Comedonica is defined by the dominant presence of non-inflammatory comedones. Unlike the red, swollen pustules and cysts associated with more severe acne forms, these lesions are typically flesh-colored, white, or dark bumps. They occur when hair follicles become clogged with a mixture of dead skin cells and excess sebum (oil).
- Open Comedones (Blackheads): These appear dark because the pore is open to the air, causing the melanin (skin pigment) and sebum within the follicle to oxidize, turning a dark color. They are not dirt, but rather oxidized cellular debris.
- Closed Comedones (Whiteheads): These are small, flesh-colored bumps that remain under a thin layer of skin. They are not exposed to air, so the contents don't oxidize, maintaining their lighter appearance.
The severity of Akne Comedonica is often graded based on the number of comedones present, particularly on one half of the face:
- Grade I: Less than 10 comedones per face half
- Grade II: 10-25 comedones per face half
- Grade III: 25-50 comedones per face half
- Grade IV: More than 50 comedones per face half
While often seen in adolescents due to hormonal shifts, Akne Comedonica can persist into adulthood. These comedones tend to concentrate in seborrhoeic zones—areas of the body with a higher density of sebaceous glands—most notably the face (especially the T-zone), but also the shoulders, upper back, and central chest. You might notice fewer, if any, inflammatory red papules or pustules, distinguishing it from other acne types. For a deeper dive into the different types of comedones and their appearance, you might find our article Decoding Akne Comedonica: Your Guide to Blackheads particularly helpful.
The Cosmetic Connection: Is Your Makeup Making You Break Out?
One of the most crucial aspects of understanding Akne Comedonica is recognizing its potential to be “cosmetic-induced.” This means that certain ingredients in your skincare, makeup, or even hair products can directly cause or worsen the formation of comedones. This specific form of acne is medically known as Acne Cosmetica or Acne Venenata.
How Cosmetics Contribute to Akne Comedonica:
- Comedogenic Ingredients: Many cosmetic ingredients have the potential to clog pores. These are termed “comedogenic.” When these substances sit on the skin, they can trap dead skin cells and sebum within the follicle, leading to the development of microcomedones, which eventually become visible blackheads and whiteheads. Common culprits include certain oils (e.g., coconut oil, cocoa butter in some formulations), waxes, and silicones, though individual reactions can vary widely.
- Irritation and Barrier Disruption: Harsh cleansers, astringents, or products with high concentrations of irritating fragrances or dyes can disrupt the skin’s natural barrier. A compromised barrier can lead to increased inflammation and abnormal shedding of skin cells, making pores more susceptible to clogging.
- Occlusion: Heavy, occlusive products, particularly those used overnight or thick foundations, can create a physical barrier on the skin, trapping sweat, oil, and dead skin cells, thereby fostering an ideal environment for comedone formation.
- Improper Removal: Not thoroughly removing makeup and sunscreen at the end of the day allows comedogenic ingredients to linger on the skin, increasing their chances of clogging pores.
Identifying cosmetic-induced Akne Comedonica requires careful observation. If your breakouts started after introducing a new product, or if they appear predominantly in areas where you apply certain cosmetics (e.g., forehead comedones from hair products, cheek comedones from blush/foundation), a cosmetic trigger is highly likely.
Diagnosing Akne Comedonica and Identifying Triggers
The diagnosis of Akne Comedonica is primarily clinical, meaning a dermatologist or skincare professional can usually identify it through a thorough visual examination of your skin. They will look for the characteristic non-inflammatory blackheads and whiteheads, noting their distribution and density. Generally, no further laboratory tests are needed unless the acne is severe, unusually persistent, or accompanied by other symptoms that might suggest an underlying hormonal imbalance or a different skin condition.
Pinpointing Cosmetic Triggers:
If you suspect your Akne Comedonica is cosmetically induced, becoming a “skin detective” is key:
- Product Audit: Review all your skincare, makeup, and even hair products. Look for terms like “non-comedogenic” or “non-acnegenic.” While these labels aren’t foolproof, they indicate the product has been tested to be less likely to clog pores. Avoid products that feel excessively heavy or greasy.
- Ingredient Check: Educate yourself on common comedogenic ingredients. Websites and apps can help you cross-reference ingredient lists. However, remember that an ingredient's comedogenicity can depend on its concentration and the overall product formulation.
- Elimination Diet (for products): If you've introduced multiple new products, try removing them one by one for a few weeks to see if your skin improves. Reintroduce them slowly to identify the culprit.
- Patch Testing: When trying a new product, especially one with a rich texture, test it on a small, less visible area of your skin (e.g., behind the ear or on a small patch of jawline) for a few days to a week before applying it all over your face.
- Professional Consultation: A dermatologist can help you analyze your current routine, identify potential problem products, and recommend alternatives. They can also offer professional guidance on managing the condition.
Effective Strategies for Managing and Preventing Akne Comedonica
Managing Akne Comedonica, especially when it’s cosmetically induced, involves a multi-faceted approach focusing on proper cleansing, targeted treatments, and mindful product selection.
1. Gentle and Effective Cleansing:
Start with a mild, pH-balanced cleansing syndet or an antibacterial cleansing gel. Products like Sebopona, Cetaphil, Eubos, or specific formulations like Lutsine Bactopur Cleansing Gel or Effaclar by La Roche-Posay are often recommended. The goal is to clean without stripping the skin of its natural oils, which can lead to irritation and further comedone formation. Cleanse twice daily, especially after wearing makeup or sweating.
2. Targeted Treatments for Comedone Reduction:
- Topical Retinoids (Vitamin A Derivatives): These are the gold standard for treating Akne Comedonica due to their potent anti-comedogenic effects. Retinoids work by promoting cell turnover, preventing dead skin cells from clogging follicles, and normalizing keratinization.
- For oily skin, isotretinoin gel (e.g., Isotrex Gel 0.05%) or tretinoin (e.g., Cordes VAS, Airol-Lösung 0.05%) used once nightly, or adapalene 0.1% gel (e.g., Differin Gel).
- For normal skin, tretinoin 0.05% cream (e.g., Cordes VAS Creme) or isotretinoin 0.05% cream.
- For sensitive skin, adapalene 0.1% gel (Differin Gel) or azelaic acid 20% (e.g., Skinoren) once nightly, as they tend to be less irritating.
- These can sometimes be combined with other actives like azelaic acid 20% or benzoyl peroxide 2.5-10% (e.g., Akneroxid Gel 5-10%) for enhanced efficacy.
Topical retinoids are also excellent for maintenance therapy, significantly reducing the recurrence of microcomedones.
- Manual Extraction: Performed by a trained professional (dermatologist or skilled aesthetician), manual extraction using a comedone extractor or a Moncorps knife can safely remove existing blackheads and whiteheads without damaging the skin. This “Acne Toilette” is a crucial step in clearing the skin.
- Antikomedogenic Gels and Cover-up Creams: During the day, gels containing ingredients like benzoyl peroxide (e.g., Akneroxid Gel 5-10%, Aknefug-oxid mild 3-10%) can help. Medicated cover-up creams (e.g., Lutsine Creme hell/gold) can conceal while also treating.
- Chemical Peels: Under professional supervision, mild chemical peels (e.g., salicylic acid or glycolic acid peels) can help exfoliate the skin and reduce comedones.
3. Mindful Product Selection and Application:
- “Non-Comedogenic” & “Oil-Free”: Prioritize products labeled as such. These formulations are designed to minimize pore-clogging.
- Mineral Makeup: Many find mineral-based foundations and powders to be less irritating and less likely to cause comedones compared to traditional liquid foundations.
- Lightweight Formulas: Opt for gels, serums, and light lotions over heavy creams, especially for facial use.
- Hygiene: Regularly clean makeup brushes and sponges to prevent the transfer of bacteria and old product residues to your skin.
- Hair Care Awareness: If you notice comedones on your forehead or temples, check your shampoo, conditioner, and styling products. Some can be surprisingly comedogenic.
When it comes to active treatment, understanding the various options is crucial. Our guide, From Retinoids to Extraction: Treating Comedonal Akne Effectively, delves deeper into these methods.
Conclusion
Akne Comedonica, characterized by its non-inflammatory blackheads and whiteheads, can significantly impact skin texture and confidence. While various factors contribute to its development, the role of cosmetic-induced acne (Acne Cosmetica) is an often-underestimated but critical piece of the puzzle. By understanding what Akne Comedonica is, recognizing the potential impact of your daily products, and adopting a proactive approach to treatment and prevention, you can pave the way for clearer, smoother skin. Always remember to prioritize “non-comedogenic” choices, maintain consistent skincare hygiene, and consult with a dermatologist for personalized advice and effective treatment plans tailored to your skin's unique needs.